Osteochondrosis is a lesion of the intervertebral discs of a degenerative-dystrophic nature, and the cervical spine is the most vulnerable part of the spinal column, which has an anatomically different structure of very close adjacent vertebrae and a weak muscle corset. Therefore, even with small additional loads on the neck, displacement of the vertebrae can occur, leading to compression of blood vessels and nerves.
And since the vertebral arteries that are involved in the blood supply to the brain pass through the holes in the transverse processes of the vertebrae in this section, pinching the vertebrae in this section or squeezing the holes by overgrown osteophytes is fraught with very serious consequences.
What it is?
Osteochondrosis of the cervical spine is a polyetiological progressive disease, which is manifested by degeneration of the intervertebral discs and dystrophy of the ligamentous apparatus of the spine.
Causes of occurrence
The main causes and prerequisites for the occurrence of osteochondrosis of the cervical vertebra are:
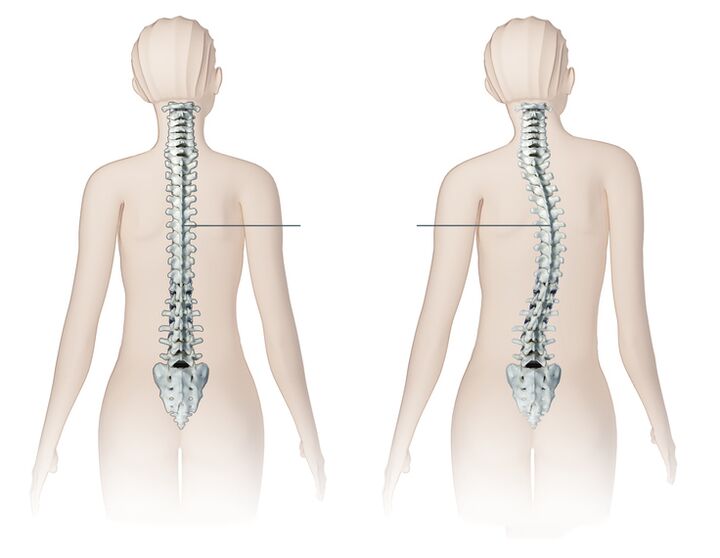
- Curvature of the spine, scoliosis.
- Stress, nervous tension negatively affect the general condition of the body, can cause cervical osteochondrosis.
- Postponed infectious diseases often become the root cause.
- Incorrect, uncomfortable body position during sleep (for example, an uncomfortable pillow).
- Congenital problems or the presence of hereditary diseases of the cervical spine.
- Poor posture in young people and adolescence.
- Overweight, obesity of various degrees. Extra pounds increase the load on the vertebrae and discs, which leads to degenerative processes.
- Back injuries that may have occurred during childhood or adolescence.
- Disruption of metabolic processes.
- Work related to physical labor, which can provoke diseases of the spine in its various parts.
- Inactive lifestyle, sedentary work, improper performance of any exercise.
For the successful treatment of cervical osteochondrosis, it is first necessary to establish the cause of the occurrence, the prerequisites that provoked its development and eliminate them. Until recently, the disease occurred only in people over the age of 45. Now young people are exposed to it, the age range is 18-25 years.
Features of the cervical spine
Consider how the cervical region differs from the rest of the spine, and that in the process of developing osteochondrosis is a prerequisite for the development of these syndromes.
- In the cervical region, there are important ganglia (nodes) of the autonomic nervous system.
- In the transverse processes of the vertebrae there are holes that form a canal through which the vertebral artery passes, which supplies oxygen and nutrients to the brain, cerebellum, hearing organs, and also the vertebral nerve. These are prerequisites for frequent artery and nerve clips.
- The cervical spine is the most mobile. He is characterized by all types of movements in full. These are prerequisites for frequent infringements and subluxations!
- The intervertebral foramen of the lower three vertebrae are not round, but triangular. These are prerequisites for the infringement of the nerve roots by bone growths, which are formed in osteochondrosis.
- The intervertebral discs are not located between the vertebral bodies along their entire length. In the front part, instead of them, there are protruding edges of the vertebrae, which are interconnected by joints.
Here are the key features from which we will build on, analyzing the symptoms and complications of osteochondrosis.
Development stages
The degree of osteochondrosis is determined by the clinical picture and the patient's complaints. The concept of degree should not be confused with the stages of osteochondrosis. The stages will be discussed below.
- First degree. clinical manifestations are minimal, the patient may complain of low intensity pain in the cervical spine, it may worsen when turning the head. Physical examination may show slight tension in the neck muscles.
- Second degree. the patient is worried about pain in the cervical spine, its intensity is much greater, the pain may be irradiating to the shoulder, to the arm. Painful sensations increase when tilting and turning the head. The patient may notice a decrease in performance, weakness, headache.
- Third degree. the symptoms of cervical osteochondrosis intensify, the pain becomes constant with irradiation to the arm or shoulder. Numbness or weakness appears in the muscles of the arm, as herniated discs form (see symptoms of a spinal hernia of the lumbar spine). Examination reveals limited mobility in the cervical spine, pain on palpation of the cervical spine.
- Fourth degree. there is a complete destruction of the intervertebral disc and its replacement with connective tissue. Dizziness intensifies, tinnitus appears, impaired coordination.
Symptoms
The severity of the symptoms of cervical osteochondrosis depends on the degree of destruction of the vertebral structures. Symptoms are aggravated by the growth of bone tissue with the formation of osteophytes, radicular syndrome (radicular pain when a nerve is pinched), intervertebral hernia (protrusion of the disc into the spinal canal).
The first signs of the disease are periodic headache in the occiput, soreness in the neck, crunching and clicks in the vertebrae when turning the head, and sometimes a slight tingling sensation in the shoulders. Over time, the symptoms increase, and the intensity of the pain increases.
Pain syndrome is the main manifestation of osteochondrosis. Pain in the neck can be dull, constant or sharp with lumbago below the occiput when turning the head. The entire cervical region or the projection area of the modified vertebra, as well as the clavicle, shoulder, scapula, and heart area, may hurt. Restriction of head movement due to pain often occurs in the morning after sleeping in an uncomfortable position.
The disease leads to compression of the roots of the peripheral nerves (radicular syndrome) and causes pain along the course of these nerves. Perhaps numbness of the hands or fingers, impaired sensitivity of certain skin areas innervated by the pinched nerve.
According to some characteristic symptoms, it can be assumed which vertebrae are affected:
- C1 - violation of sensitivity in the occipital region;
- C2 - pain in the occipital and parietal regions;
- C3 - decreased sensitivity and pain in the half of the neck where the spinal nerve was infringed, possibly impaired sensitivity of the tongue, speech impairment due to loss of control over the tongue;
- C4 - impaired sensitivity and pain in the shoulder-scapular region, decreased tone of the muscles of the head and neck, possible respiratory disturbances, pain in the liver and heart;
- C5 - pain and impaired sensitivity in the outer surface of the shoulder;
- C6 - pain extending from the neck to the scapula, forearm, outer surface of the shoulder, radial surface of the forearm to the thumb of the hand;
- C7 - pain spreading from the neck to the scapula, the back of the shoulder, the forearm to the II – IV fingers of the hand, impaired sensitivity in this area.
- C8 - pain and sensory impairment spread from the neck to the shoulder, forearm to the little finger.
Clicks or crunching during neck movements almost always accompany cervical osteochondrosis, observed in every patient. The crunch appears during a sharp turn of the head or throwing it back.
Syndromes due to cervical osteochondrosis
Symptoms of cervical osteochondrosis are grouped into specific groups called syndromes. Their presence and severity may indicate a pathology in the cervical spine with a specified localization.
A group of common syndromes:
- Vegetative-dystonic syndrome. Subluxation of the first vertebra of the cervical spine with displacement can lead to the development of vegetative-vascular dystonia. VSD is not a definite diagnosis, since it does not have pronounced symptoms. There may be neurological signs, symptoms of impaired cerebral blood flow, surges in intracranial pressure, muscle spasms. As a result, the patient's complaints are reduced to dizziness, decreased visual acuity, loss of consciousness, headaches, and nausea.
- Irritative and reflexive. Burning and sharp pain in the back of the head and neck, sometimes with a return to the chest and shoulder, arising at the time of a change in the position of the head and neck, with sneezing and a sharp turn of the head.
- Radicular. Otherwise called cervical radiculitis, it combines symptoms associated with infringement of the nerve roots of the cervical vertebrae. Characterized by "chills" in the affected area, tingling in the fingers, forearms, pasty skin, spreading to certain fingers.
- Cardiac. Almost the same picture with angina pectoris often leads to incorrect diagnosis and treatment. The syndrome appears due to irritation of the phrenic nerve receptors, partially capturing the pericardium and pectoralis major muscle. Thus, spasms in the heart area are more reflex, like a response to irritation of the cervical nerves.
- Vertebral artery syndrome. It develops directly both with compression of the artery itself, and with irritation of the sympathetic nerve plexus, which is located around it. The pain in this pathology is burning or throbbing in the occipital region with spread to the temples, superciliary arches, crown. Occurs both on one and both sides. Patients usually associate exacerbation with the state after sleeping in a non-physiological position, traveling in transport, walking. With severe symptoms, hearing loss, dizziness, tinnitus, nausea, vomiting, loss of consciousness, increased blood pressure are possible.
The nonspecificity and a large number of various symptoms accompanying this disease complicate the diagnosis and further treatment, since some of them may be a sign of completely different diseases.
Diagnostics
As with any diagnosis in medicine, the diagnosis of osteochondrosis is established on the basis of the patient's complaints, medical history, clinical examination and auxiliary research methods. Radiography of the cervical spine is performed in frontal and lateral projections, if necessary in special positions (with an open mouth). At the same time, specialists are interested in the height of the intervertebral discs, the presence of osteophytes.
Of the modern research methods, NMR and CT studies are used, which allow the most accurate verification of the diagnosis. In addition to the listed methods of additional research, you may need to consult related specialists (cardiologist, ophthalmologist, neurosurgeon), and examination by a neurologist is simply vital. A neurologist is involved in the treatment of osteochondrosis, therefore, after examining the patient, he, at his discretion, will prescribe the necessary minimum examination.
How to treat osteochondrosis of the cervical spine?
Complex treatment of cervical osteochondrosis can include the following traditional and non-traditional methods: drug treatment, massage, acupressure, manual therapy, physiotherapy, acupuncture, homeopathy, folk remedies, etc.
The main treatment regimen for osteochondrosis is the same for all localizations of this disease:
- First you need to relieve pain.
- Then the swelling will be removed.
- At this stage, it is necessary to normalize blood circulation.
- Strengthening the muscle corset.
- Improving nutrition and tissue regeneration.
The list of medicines and drugs for the treatment of cervical osteochondrosis at home is very extensive:
- Anti-inflammatory (steroid). These are hormonal drugs that relieve inflammation and, thereby, eliminate pain. Most often, for osteochondrosis of the cervical spine, tablets and ointments are used based on the substances of hydrocortisone, prednisolone or dexamethasone;
- Analgesics (non-steroidal pain relievers). They are usually prescribed as tablets or capsules. It should be remembered that most of these drugs irritate the lining of the digestive tract. Among the modern drugs used to relieve pain in osteochondrosis;
- Muscle relaxants are drugs that relax muscle tone. They are used in surgery and orthopedics as aids to relieve pain. These medications are administered parenterally, and therefore always under the supervision of a physician. There is an extensive list of contraindications;
- Chondroprotectors are preparations containing substances that replace the components of cartilage tissue - chondroitin, hyaluronic acid. To achieve a lasting positive effect, such drugs must be taken for a very long time;
- Ointments and gels for external use. This is the most accessible group of drugs for use at home. They are divided into relieving inflammation, warming and pain relievers. Such funds are often advertised. With cervical osteochondrosis, not all ointments are effective, in addition, due to their availability, they are sometimes used unreasonably and without taking into account the peculiarities of pathogenesis.
- Vitamins. With osteochondrosis, vitamins are prescribed, which have a beneficial effect on the peripheral nervous system and improve conductivity. Water-soluble vitamins: B1, B6, B12, fat-soluble vitamins: A, C, D, E. In recent years, it has become more common to prescribe combined preparations containing both painkillers and vitamin components. An effective preparation consists of B vitamins based on pyridoxine and thiamine, as well as an anesthetic.
Only a team of good specialists can choose the most suitable therapy, which includes a neurologist, physiotherapist, massage therapist, surgeon, and vertebral neurologist.
Physiotherapy
Exercise therapy for cervical osteochondrosis should be carried out outside of acute exacerbation. The greatest efficiency of this technique is during the recovery period. There should be no discomfort and pain during the execution of the complex!
- Exercise # 1 Lying on your stomach, put your hands on the floor, raise your head and torso, your back should be straight. Remain in this position for 1-2 minutes. Slowly lower yourself to the floor. Repeat 2-3 times.
- Exercise number 2 Lying on your stomach, stretch your arms along the body, turn your head to the left, try to touch the floor with your ear, then turn your head to the right. Repeat 6-7 times in each direction.
- Exercise number 3 In a sitting position, while inhaling, bend forward, and try to touch your chest with your head, then exhaling, bend back and tilt your head back. Repeat 10-15 times.
- Exercise # 4 Sitting place your palms on your forehead, apply pressure with your palms on your forehead, and your forehead on your palms. Continue this exercise for 30 seconds. Repeat 2-3 times.
- Exercise number 5 Slowly rotate your head first in one direction, then in the other direction. 10 rotations in each direction. Watch for dizziness. When it appears, the exercise stops.

Massotherapy
Massage can be performed at home, but very carefully so as not to aggravate and harm the patient. The patient should take a supine position, put the forehead on the hands and stretch the chin towards the chest. In this case, the muscles of the neck should be completely relaxed.
- Stroking. It is necessary to start the massage with these movements: stroking the collar zone in the direction from the lymph to the supraclavicular and axillary nodes. Then flat and comb-like strokes are applied.
- Push-ups. To perform push-ups, the masseur places a hand across the neck (index and thumb should be together) and moves down the spine. Also push-ups can be performed with the edge of the palm up to the shoulder joints.
- Trituration. Rubbing is done to warm up the muscles, relax them, and improve blood flow to the area. Massage should begin from the base of the skull, performing circular and rectilinear movements with your fingers. You can also perform sawing movements with palms parallel to the ribs.
- Kneading. Kneading should be performed on the neck in a circular motion.
- Vibration. The massage ends with stroking and vibration, which is performed with the help of shaking and tapping.

Massage is necessary to strengthen muscle tone and relieve pain. Depending on the stage at which osteochondrosis is, a massage technique is selected. Nevertheless, when doing neck massage, specialists use all the techniques of classical massage: rubbing, stroking, kneading, etc. In cases where the patient has a pain in the neck area only on one side, the massage begins in the healthy part of the neck, gradually moving to that part of the collar zone where strong painful sensations arise.
Manual therapy
Manual therapy helps to cope with both acute and chronic pain, it also increases the range of motion and improves posture well. The main methods of manual therapy for osteochondrosis of the cervical spine:
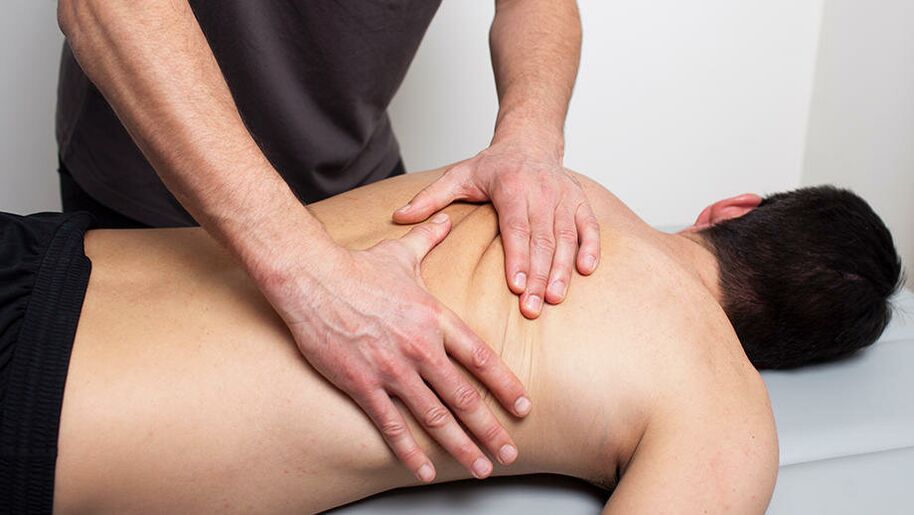
- Relaxing and segmental massage. It is used to warm up muscles and relieve tension.
- Mobilization. Effects aimed at restoring the functions of the joints. traction method.
- Manipulation. A sharp push aimed at the pathological areas of the patient. The procedure is accompanied by a characteristic crunch (return of the joint to its normal position).
A specialist practicing manual therapy should be fluent in these techniques. Otherwise, any mistake can lead to injury.
Orthopedic pillows

Orthopedic sleep pillows are an effective preventive measure. In many cases, osteochondrosis is aggravated by additional compression of the cervical artery and nerve roots while sleeping on an uncomfortable pillow. The orthopedic product ensures a uniform horizontal position of a person during sleep and, thereby, guarantees a physiologically adequate blood supply to the brain.
When choosing a pillow, one should take into account the individual anatomical features of a person and correlate them with the volume and characteristics of the filler. A correctly selected pillow brings tangible benefits to a patient with osteochondrosis of the cervical spine.
Physiotherapy
Physiotherapy procedures for cervical osteochondrosis:
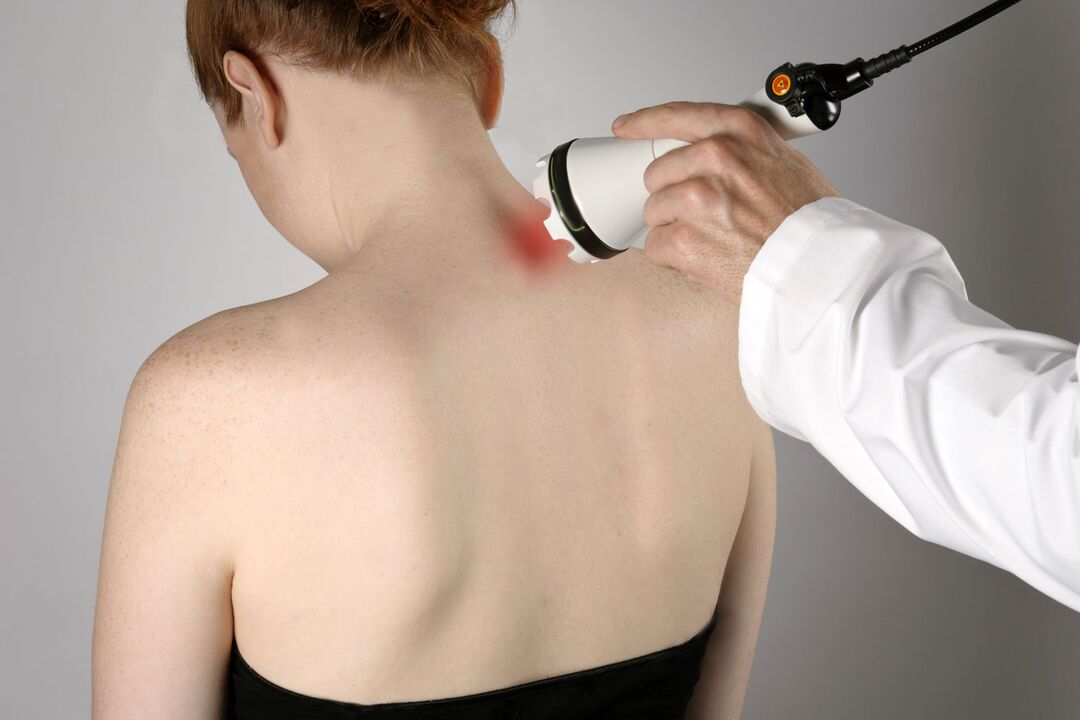
- Electrophoresis. Should be used with pain relievers (anesthetics), which are injected under the skin by means of electronic pulses
- Ultrasound. It has a beneficial effect on metabolic processes in the tissues of the cervical spine, due to which puffiness is removed, pains go away.
- Magnetotherapy. A safe method of treatment, which consists in exposing damaged cells to a low-frequency magnetic field. It gives an analgesic effect, acts as an anti-inflammatory agent
- Laser therapy. Improves blood circulation in the affected area, relieves tissue swelling, pain.
Physiotherapy procedures have a beneficial effect on discs and vertebrae in cervical osteochondrosis. In combination with taking medications, combined treatment helps to get rid of the symptoms of the disease. The procedures are carried out in a hospital or specialized offices at polyclinics. Before starting the course, you must consult a doctor, determine the duration of physiotherapy, types. It is strictly forbidden to pass it during an exacerbation.
Shants Collar
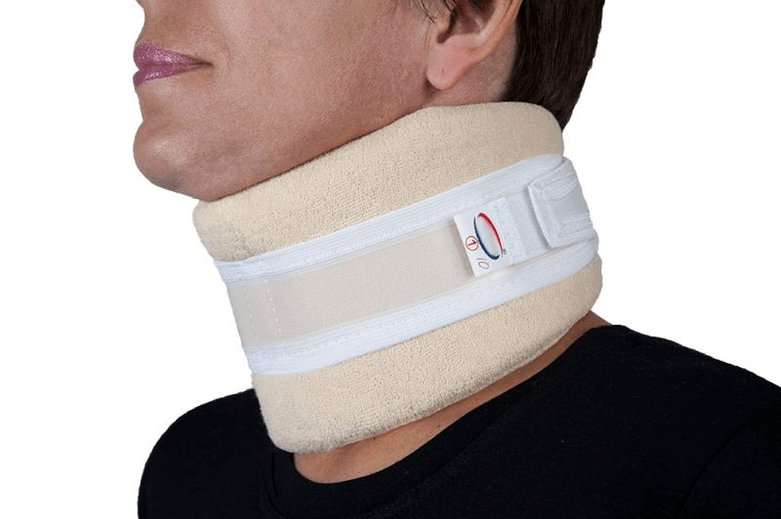
The Shants collar is a soft and comfortable device that fastens with Velcro at the back and is used for cervical osteochondrosis. But not for treatment, but for temporary relaxation and relieve fatigue. It cannot be worn without taking it off, otherwise the neck muscles will stop working and soon atrophy. If the collar of Shants is chosen correctly, the patient feels comfortable and protected.
The collar is selected strictly according to the size in the pharmacy or orthopedic store. Better in the store, because the people who work there, as a rule, know their business and the characteristics of the product quite well, which means they can help in each specific case.
Folk remedies
If the pain from osteochondrosis of the spine becomes unbearable and regular, then you will agree to anything to stop it, and here traditional complex treatment will be successfully complemented by alternative methods.
- insist celery root (5 grams per 1 liter of boiling water) for 4 hours, drink a tablespoon before each meal;
- honey compress, for which we take 2 tsp. honey and 1 tablet of mummy. We heat the components in a water bath, spread on a cloth and apply to the cervical region, that is, the neck, at night;
- in case of acute pain, horseradish growing in the country helps me. I just wash his leaf, pour it over with boiling water, cool it a little, apply it to the neck and wrap it with a thin scarf for the night - in the morning you can already live and work;
- we insist chamomile flowers in vegetable oil for two days, preheating to a boil (for 500 ml of oil, 30 grams of a plant are needed), rub into sore areas;
- honey-potato compress also helps, for this, the root crop must be grated and mixed with honey in the same amount, applied to a large neck at night, used regularly, at least once a week.
Prophylaxis
As usual, proper prophylaxis will help to avoid osteochondrosis of the cervical spine, but, of course, all physical exercises must be used regularly, otherwise there will not be much benefit from "periodic" exercises.
It remains to remember simple rules:
- eat more foods with a lot of calcium and magnesium. These are fish, peas, legumes, nuts, cheese, herbs, but it is better to refrain from sugar, flour, smoked, spicy foods.
- regularly go in for sports, especially swimming, water aerobics, and gymnastics for stretching and flexibility of the vertebrae is also suitable to prevent osteochondrosis, which can be practiced at home.
- during sedentary work, at least a couple of times a day, perform a special set of exercises, an example of which is in the video.
- choose a good orthopedic mattress and a pillow that is ideal for the neck, supporting the head in a dream in the correct anatomical position (yes, your favorite huge down pillows will not go away with problems with the spine! ).
If you already have such a diagnosis, then the patient should spare his spine, namely:
- Be very careful with lifting and carrying weights, it is better to go to the store twice than to pull heavy bags in both hands, incredibly straining your neck and shoulder girdle;
- Do not overcool, avoid drafts and the flow of cold air from the air conditioner (some people like to cool down on a hot day, standing with their backs to the fan);
- When bending the body forward - remember about osteochondrosis;
- Avoid local overheating of the muscles, which can happen to those who like an excessively hot bath;
- Do not forget to periodically break away from the monitor, change the position of the body, do not sit for hours, or even days;
- Rest your neck, for which you need to purchase a Shants collar;
- If possible, if the condition of the cardiovascular system allows, take a steam bath.
In conclusion, I would like to say that a child who is at risk of osteochondrosis (the father and mother already have it) and an adult who acquired the disease in the course of life are simply obliged to take preventive measures so as not to become disabled and not be on the operating table, because this operationrather difficult and requires long-term rehabilitation. In addition, it is not always possible, because there are inoperable cases, so it is better to protect health from a young age, as long as the discs are intact and unnecessary growths do not squeeze the blood vessels.





















